Lebanon, a small country of nearly 6 million people, is navigating one of its most difficult periods in recent years. Escalating conflict in the Middle East has spilled into Lebanon, displacing more than 1.2 million people, of whom approximately 350,000 are children. The fighting has damaged homes and critical civilian infrastructure, restricting access to such essential services as healthcare, mental health and psychosocial support (MHPSS), protection services, schooling, and water and sanitation. The health system is under immense strain—because of the conflict, six hospitals and 46 primary healthcare centres (PHCCs) remain non-operational.
Anil Kangal, International Medical Corps Country Director in Lebanon, is leading our efforts to support affected communities. Kangal has been serving in her current role since May 2024, but her tenure goes back to 2014, when she joined International Medical Corps as deputy programme manager in Türkiye. Since then, she has held different positions in various countries, including Djibouti, Ethiopia, Libya and Tunisia. Today, she oversees the Lebanon mission’s strategic direction, humanitarian programming and emergency response, leading a multi-sector portfolio that supports populations affected by multiple crises in the country, including Syrian refugees and Lebanese and migrant workers.

In this interview, she discusses the growing humanitarian needs in Lebanon, the challenges of providing care there and the resilience of our teams and communities.
Can you please give us a quick overview of the situation in Lebanon and the needs there, and talk about how we are responding?
Lebanon continues to face a severe and fast-moving humanitarian crisis. Despite the temporary ceasefire and the ongoing negotiations, attacks continue, especially in southern Lebanon. This is causing widespread destruction, displacement and enormous pressure on an already fragile public system. The health system here is under immense strain due to mass casualties, repeated attacks on health infrastructure and supply shortages.
We’re responding in close coordination with the Ministry of Public Health (MoPH) and other partners through the PHCCs we support and the mobile primary satellite units (PSUs) that are providing consultations, medicines, vaccinations, referrals, hygiene items, nutrition support and MHPSS across various shelters and displacement sites. So far, we have supported 115 shelters and provided more than 10,000 consultations for the displaced populations.
Children make up a large portion of the displaced population. How are our teams helping children and parents feel safe and cared for amid all the uncertainty?
About 350,000 of the displaced population includes children, who carry a huge burden of this crisis. Many of them live in overcrowded shelters with limited privacy, interrupted schooling and high levels of stress. We’re trying to provide them with care and reassurance in these uncertain times.
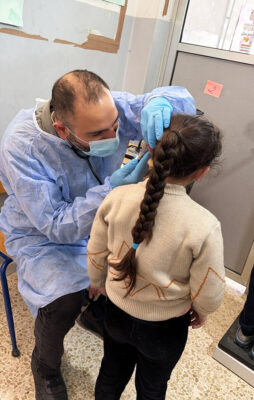
Through our PSUs, we provide primary healthcare consultations, medications for acute and chronic illnesses, routine vaccinations, nutrition screening, referrals and health-awareness sessions. We also provide MHPSS services, which are critical not only for children but also for parents trying to keep their families together under pressure. Even basic interventions—such as hygiene kits and health education—can help families feel more dignified, safe and better supported in shelters.
Being pregnant in a war zone comes with its own challenges. How are we supporting expectant and nursing mothers?
Pregnant and breastfeeding women face some of the most acute risks in the ongoing crisis. According to the World Health Organization, about 325,000 women of reproductive age make up the displaced population—and 13,500 of them are pregnant, with roughly 1,500 of them expected to give birth within a month. These women are living in overcrowded shelters with poor sanitation, and their access to routine maternal care has been disrupted.
So, our teams are supporting pregnant and breastfeeding women through screening and nutrition support. So far, we have reached more than 600 children under 5 and pregnant and breastfeeding women, providing them with essential nutritional supplementation. Our PHCCs and PSUs are also making referrals for these women and children, to ensure continuity of care. This is critical in a setting where attacks on healthcare infrastructure, as well as supply shortages, are disrupting access to lifesaving maternal care.
“Many of our staff are serving people whose experiences they understand first-hand. Our dedicated teams are focused on delivering service in challenging conditions because they know what it means for people in shelters to see a trusted healthcare worker arrive.”

Mental health needs often increase during crises like this. In addition to the medical needs, what are you seeing in terms of emotional and psychological needs?
The emotional and psychological toll is enormous because, over the past couple of years, Lebanon has endured a number of multi-layered crises. People had already been living with repeated displacement, fear, grief, uncertainty and economic stress. Children are showing clear signs of emotional turmoil, and women and caregivers are under intense pressure in overcrowded shelters, where they have little or no privacy. We’re seeing a lot of anxiety, distress and sleep disruption.
That is why, in addition to providing medicines, consultations and primary healthcare, we’re providing MHPSS, working with the National Mental Health Program. So far, we have reached more than 500 people with psychological first aid and non-specialised support, alongside more structured case management and specialised care, delivered both remotely and in person.
Nearly every part of Lebanon’s health system is feeling the strain right now. What does that pressure look like on a typical day for our staff and PSUs working in shelters and communities?
On a typical day, we see massive needs in a system that is already overstretched. Health facilities have been damaged or forced to close, while the supply chain has been disrupted. Our staff and PSUs are working in shelters and communities where people may have fled with almost nothing. We see people arriving with urgent needs, including needs for chronic-disease management, maternal health services, mental health support and routine vaccinations for children.
Our teams are working hard to address these gaps while dealing with their own personal challenges—about 25% of our staff have been displaced—but they continue to show up for their communities. They’re trying to maintain continuity of care in hard-to-reach areas while adapting to security and access constraints, as well as the constant possibility that needs may surge again rapidly.
“In difficult conversations with families, what stays with me is not only the scale of their loss but the dignity and strength they bring into their uncertainty. That combination of suffering, loss, responsibility and resilience is something you do not forget.”
As you mentioned, the ongoing conflict has displaced many of our staff. What do you think motivates them to show up every day despite personal challenges?
In the context of Lebanon, the term “resilience” is very human. It is our staff continuing to serve others while they themselves may be worried about their families. Our dedicated teams focus on service delivery in challenging conditions because they know what it means for people in shelters to see a trusted healthcare worker arrive. And I think what motivates them is a mix of professional commitment, solidarity and a deep sense of responsibility to their communities.
Many of our staff are serving people whose experiences they understand firsthand. And in a crisis like this, that connection really matters, because it creates empathy and determination. We also feel proud to be able to offer lifesaving support even in very unstable conditions. Despite the operational strain and personal challenges, International Medical Corps has maintained operations, all our staff members are safe, and our teams continue to provide services at scale.

When you speak with families who have been affected, what stays with you most about their stories?
What stays with me the most is how suddenly everything can change for a family, and yet how determined people are to protect one another. Many families have fled with almost nothing. Some have been displaced more than once, and continue to be displaced. Parents are trying to comfort their children in unfamiliar settings while worrying about basics like food, medicine and schooling. They don’t know what tomorrow will bring, yet they make the best of each day. So what stays with me is not only the scale of their loss, but the dignity and strength they bring into their uncertainty. Even in very difficult circumstances, families focus not only on what they need for themselves, but on how to keep children safe, how to care for older relatives or how to regain a sense of stability that has been missing for so long. That combination of suffering, loss, responsibility and resilience is something you do not forget.
Looking ahead, what gives you hope as International Medical Corps continues its work in Lebanon? What would you want people around the world to understand about the needs—and strengths—of communities there?
What gives me hope is the strength of communities and the fact that, even in this difficult context, the local systems and humanitarian teams are still functioning, adapting and responding to the constantly evolving situation. I also draw hope from the commitment of our frontline staff, from the coordination with the MoPH and other partners, and from the fact that our timely support can make a real difference.
I’d like people around the world to understand that the needs in Lebanon are both urgent and complex. It’s not just about trauma care. It’s about displacement, chronic diseases, maternal health, child well-being, mental health, nutrition and dignity. We also need to realise that the communities here are not passive victims. They’re showing extraordinary strength under very difficult circumstances. What they need is sustained support, protection and resources to keep at least the essential services running.
Learn more about our lifesaving work in Lebanon, or read the latest situation report about our response to the conflict in the Middle East.
