The military-political crisis that broke out in 2012 has severely crippled the healthcare system in the Central African Republic (CAR). This is especially true when it comes to mental health services. Stigmatization and misunderstandings about the causes of mental health issues and the effectiveness of treatment at the community level also impede necessary care.
According to the World Health Organization, the prevalence of mental disorders increases significantly in the context of humanitarian crises—yet in countries such as CAR, coping with an already weakened healthcare system, the need to provide mental health services is often overlooked. As such, where mental health and psychosocial support services (MHPSS) are needed the most, they are often hard to come by.
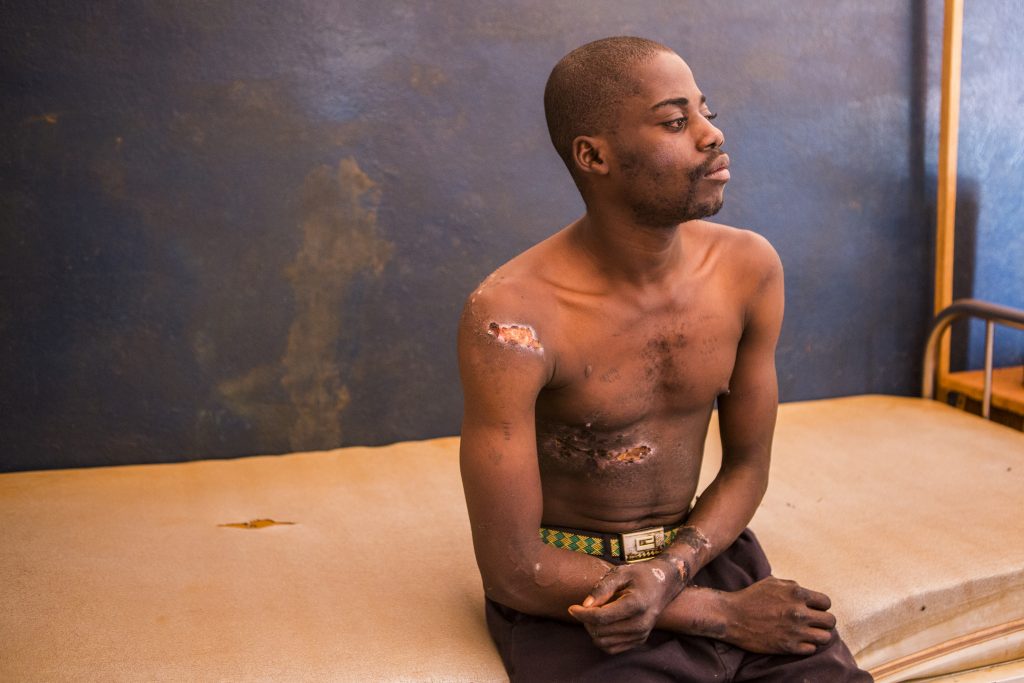
23-year-old Isaï was raised in the village of Yakada, 10 kilometers away from the city of Bria. Forced to leave his home due to conflict in Yakada, he and his mother now reside outside of the village, with farming as their main source of income.
Isaï first came to Bria Hospital in March 2018 on the back of a motorcycle. His mother had heard about the free health services that International Medical Corps provides in the hospital, encouraged her son to seek treatment and brought him to the hospital. As a result of extreme agitation, the young man had been tied up for at least 10 days. Severely dehydrated, he had been unable to sleep or eat. His wounds had become deeply infected and he needed immediate care.
Isai received vital care from an ER nurse, who recognized signs of mental disorder, thanks to the MHPSS training she had received from International Medical Corps. The International Medical Corps psychiatrist at the hospital diagnosed Isaï with psychosis and epilepsy. With treatment and medication, Isaï’s condition stabilized—and after only two days of treatment, he felt well enough to eat again.

Isaï was discharged from the hospital 10 days later but returned to the hospital every two weeks for follow-up visits. He developed a good relationship with his psychiatrist, who encouraged him to continue his medication and follow-up visits. During the first two visits, Isaï’s mother accompanied him to the hospital but he soon felt well enough to visit the hospital on his own.
Today, Isaï eats and sleeps well. He takes care of himself and can work in the fields again. Having relied on assistance to get around, he now manages to get from one place to another by himself. He is grateful for the help International Medical Corps provided to him, and for the training it provided to the nurse who treated him. Isaï now hopes to get married in the future, and wants to take care of his mother—as she once took care of him.

Lacking the means to pay for treatment, Isaï was only able to access adequate mental health services because this assistance was provided free of charge. Thanks to EU Trust Fund for the Central African Republic Bêkou, International Medical Corps continues to provide mental health services in the community, working alongside nurses and primary healthcare workers who provide vital MHPSS services to those who need it the most.
To learn more about our Mental Health Integration programming in CAR, please read a recent article written by our staff, “Integrating mental health into primary healthcare in the Central African Republic” in the special feature of Number 72 July 2018 Humanitarian Exchange Magazine. Additionally, a panel presentation highlighting this work was held by Overseas Development Institute; a recording can be found here: Improving mental health care in humanitarian crises.
